
“The Pill That Fights Mosquitoes from the Inside Out”
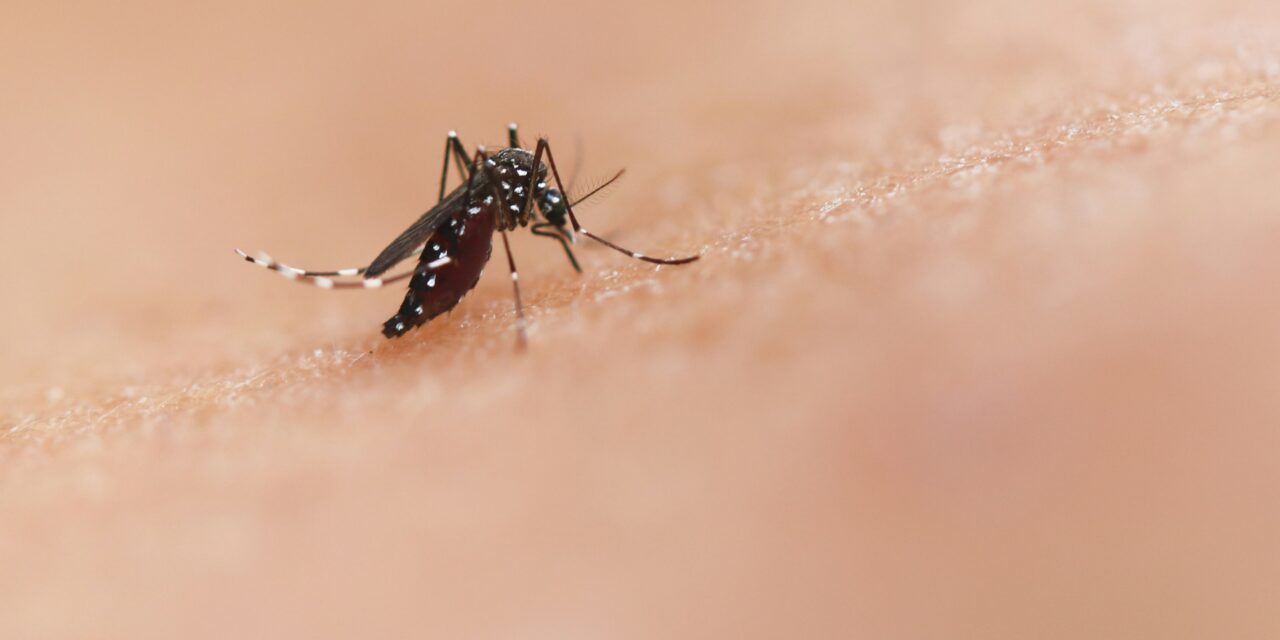
Mosquitoes are more than just a summertime nuisance — they are some of the deadliest creatures on Earth. Each year, millions of people suffer and die from mosquito-borne diseases like malaria, dengue fever, Zika virus, and yellow fever. In fact, the World Health Organization (WHO) estimates that malaria alone kills over 600,000 people annually, most of them children in sub-Saharan Africa. But now, a groundbreaking new approach might turn the tide in this ongoing war — a drug that turns your blood into a mosquito killer.
Imagine a simple pill that not only protects you from mosquito bites, but also kills the mosquitoes that bite you. That’s exactly what scientists are working on, and early results are both exciting and promising. In this blog, we’ll explore how this revolutionary drug works, the science behind it, and what it could mean for global health in the future.
The Mosquito Problem: A Global Health Crisis
Mosquitoes are not just annoying insects — they are vectors for some of the most dangerous diseases known to man. Malaria, spread by the Anopheles mosquito, has plagued humanity for centuries. Dengue, chikungunya, Zika, and yellow fever are also transmitted by Aedes mosquitoes. These diseases are particularly devastating in tropical and subtropical regions, where access to healthcare and mosquito control measures are limited.
Conventional methods of mosquito control include insecticide-treated bed nets, indoor spraying, larvicides, and public sanitation. While effective, these measures are often difficult to implement consistently in low-resource settings. Moreover, mosquitoes are developing resistance to many commonly used insecticides, making it harder to control their populations.
The Breakthrough: Turning Humans Into Mosquito Traps
The new drug, called ivermectin, isn’t new at all — it’s been around for decades. Originally used to treat parasitic infections in humans and animals, ivermectin has shown a surprising secondary effect: it’s lethal to mosquitoes when they ingest it through a human blood meal.
In recent years, researchers have begun investigating ivermectin as a “mosquitocidal” agent. When a person takes the drug, it stays in their bloodstream for several days. During this period, if a mosquito bites that person, the drug enters the mosquito’s system and kills it — often within 24 to 48 hours.
This approach turns each medicated human into a walking mosquito trap. Instead of just preventing mosquito bites (like with repellents or nets), the medicated person actually helps reduce mosquito populations by killing the insects that bite them.
How It Works: The Science of Ivermectin
Ivermectin works by interfering with the nervous system of .invertebrates It binds to certain chloride channels in nerve and muscle cells, causing paralysis and death in parasites and insects. Humans and other vertebrates don’t have these specific receptors, which is why the drug is safe when used at appropriate doses.
When used for mosquito control, ivermectin is administered in doses that are safe for humans but high enough to kill mosquitoes that feed on their blood. In clinical trials and field studies, researchers have shown that a single dose can make a person’s blood lethal to mosquitoes for up to 14 days.
Importantly, this doesn’t just kill adult mosquitoes — it also disrupts the life cycle of disease transmission. If a mosquito bites a person who has malaria but dies before it can bite someone else, the parasite has no chance to spread. This breaks the chain of transmission and can significantly reduce the disease burden in entire communities.
Real-World Trials: Promising Results from Africa
@ehsanbajwapk
ضلع بہاولنگر والوں کے لئے خوشخبری
♬ original sound – Ehsan Ul Haq Bajwa
Field trials of ivermectin-based mosquito control are already underway in parts of sub-Saharan Africa, where malaria is endemic. One such study, known as the BOHEMIA project (Broad One Health Endectocide-based Malaria Intervention in Africa), is testing mass drug administration of ivermectin in Mozambique and Tanzania.
The strategy is simple: give ivermectin to large portions of the population — including livestock, which mosquitoes also bite — and monitor the effects on mosquito populations and malaria transmission. Early results have shown a significant drop in mosquito survival rates and a reduction in malaria cases.
Another study in Burkina Faso, published in The Lancet Infectious Diseases, showed that ivermectin reduced the number of malaria-infected children by nearly 20% in villages where it was distributed. The drug was well tolerated, and adverse effects were minimal, confirming its safety for large-scale use.
Potential Advantages Over Traditional Methods
@abubakarbrand48 #foryoupage #viral ♬ original sound – Attractive Boy
There are several key reasons why this approach is so promising:
-
Targeted Impact on Mosquitoes: Instead of trying to spray entire regions with insecticides, ivermectin targets mosquitoes at their most vulnerable — during feeding.
-
Works Even in Hard-to-Reach Areas: Insecticide-treated nets and indoor spraying rely on infrastructure and compliance. Ivermectin can be delivered via pills, making it easier to deploy in remote areas.
-
Dual Benefit: Ivermectin also treats parasitic infections like river blindness and lymphatic filariasis, meaning it provides multiple health benefits with a single treatment.
-
Reduces Transmission: By killing mosquitoes before they can spread disease, the drug may help suppress outbreaks and prevent epidemics.
Challenges and Considerations
Despite its promise, this approach isn’t without challenges. For one, repeated dosing may be necessary to maintain effectiveness, especially in high-transmission seasons. Mass drug administration programs must be carefully managed to avoid overuse, which could potentially lead to drug resistance — both in parasites and mosquitoes.
There are also regulatory hurdles. While ivermectin is already approved for human use, using it as a mosquito-control strategy would require additional testing and approvals in many countries. Questions around dosing schedules, cost-effectiveness, and long-term ecological impacts need to be addressed.
Ethical concerns also arise: who decides who gets treated? Should entire communities be medicated, even if some individuals don’t want the drug? Balancing public health with individual autonomy will be critical in designing fair and effective programs.
The Future: A New Weapon in Our Arsenal
As global health agencies continue to battle malaria and other mosquito-borne illnesses, innovative tools like ivermectin offer fresh hope. Used in combination with existing strategies — such as bed nets, vaccines, and environmental controls — this drug could become a vital part of integrated disease management plans.
Even more exciting, researchers are exploring other drugs with similar mosquitocidal properties, as well as genetically engineered mosquitoes that can’t transmit disease. The idea of fighting mosquitoes from the inside out — literally weaponizing our own blood — represents a paradigm shift in disease control.
Final Thoughts
The idea of turning human blood into a mosquito killer sounds like science fiction, but it’s rapidly becoming science fact. With ongoing research, community engagement, and careful implementation, drugs like ivermectin could help protect millions from deadly diseases and reduce the global burden of mosquito-borne illnesses.
It’s not a silver bullet — but in a world increasingly threatened by climate-driven disease outbreaks and insecticide resistance, this new approach offers a powerful and unexpected ally in the fight against one of humanity’s oldest foes.






